The healthcare and insurance industries are undergoing rapid digital transformation, and in 2026, technology plays a critical role in improving operational efficiency, customer experience, and regulatory compliance. Health insurance providers are increasingly adopting advanced software solutions to streamline processes such as policy management, claims processing, underwriting, and customer engagement.
Health insurance software development focuses on building secure, scalable, and intelligent platforms that simplify complex insurance workflows. These solutions enable insurers to reduce manual errors, improve decision-making, and deliver personalized services to policyholders.
With rising healthcare costs, increasing policyholder expectations, and strict regulatory requirements, investing in robust health insurance software is no longer optional—it is essential for staying competitive in a fast-evolving market.
Market Stats
The health insurance software market is experiencing strong growth due to increasing digital adoption and demand for automation.
📊 Market Size & Growth
- The health insurance software market was valued at around $15 billion in 2025 and is projected to grow steadily beyond $26 billion by 2031.
- The broader insurance software market is expected to reach $20.41 billion by 2031, growing at a CAGR of 6.31%.
- Health insurance tech market is projected to grow from $7 billion in 2025 to $12.1 billion by 2032.
📈 Key Growth Drivers
- Rising demand for automation in claims and policy management
- Increasing adoption of cloud-based insurance platforms
- Integration of AI for fraud detection and risk assessment
- Growing need for digital customer experience
🌍 Regional Insights
- North America dominates due to advanced healthcare infrastructure
- Europe follows with strong regulatory frameworks
- Asia-Pacific is the fastest-growing region due to rising insurance penetration
🔮 Future Trends
- AI-driven underwriting and claims processing
- Integration with telemedicine and wearable devices
- Real-time analytics and predictive insights
Core Features
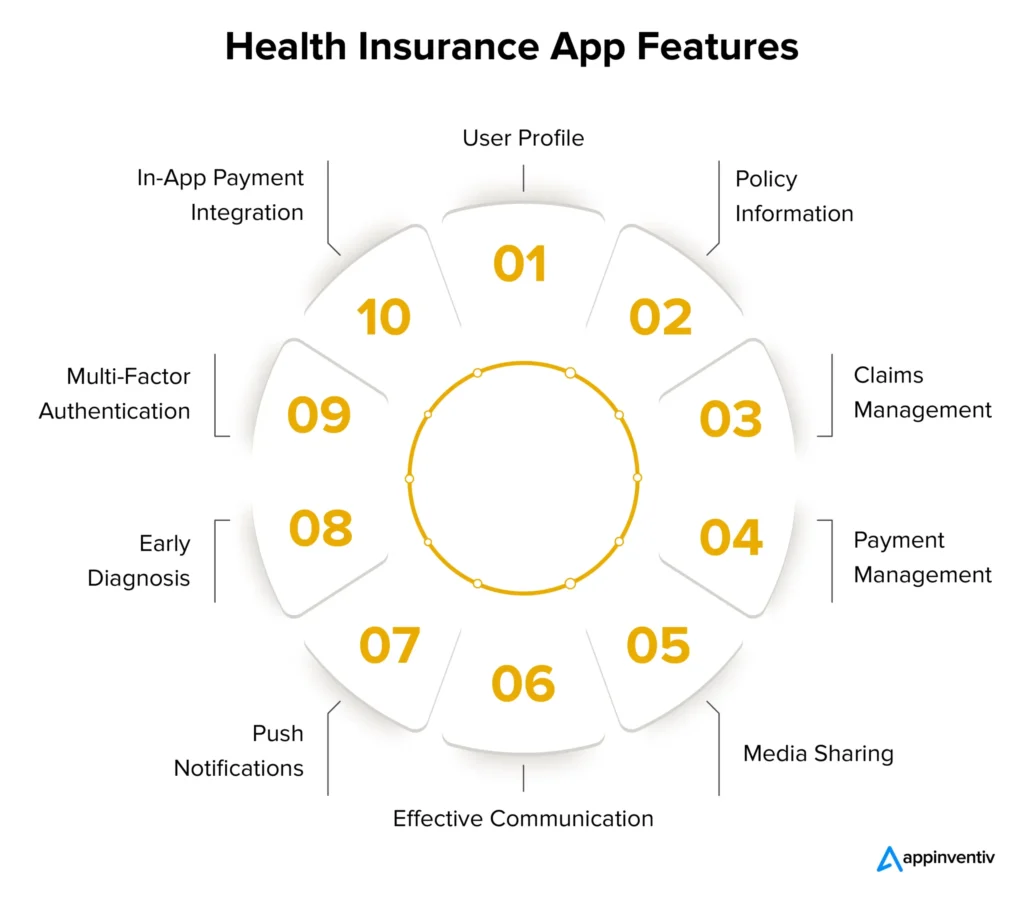
Health insurance software is built on a set of core features that ensure smooth operations, regulatory compliance, and a seamless experience for both insurers and policyholders. These foundational capabilities are essential for managing complex insurance workflows efficiently and accurately.
👤 User & Policy Management
User and policy management is the backbone of any health insurance platform. It enables users to register, create profiles, and manage their insurance policies with ease. Administrators can create, update, and manage various policy plans, including coverage details, premiums, and renewal schedules.
This feature also allows policyholders to:
- View policy details
- Update personal information
- Renew or upgrade plans
Why it matters:
Simplifies policy lifecycle management and improves customer experience.
📄 Claims Management System
Claims management is one of the most critical components of health insurance software. This feature automates the entire claims process—from submission to approval and settlement. Users can submit claims digitally, upload necessary documents, and track claim status in real time.
Advanced systems also include:
- Automated claim validation
- Fraud detection checks
- Faster claim approvals
Why it matters:
Reduces manual errors, speeds up processing, and enhances transparency.
💳 Billing & Payment Integration
This feature handles premium calculations, billing cycles, and payment processing. Integration with secure payment gateways enables users to pay premiums online through multiple methods such as cards, net banking, or digital wallets.
Key capabilities include:
- Automated billing reminders
- Invoice generation
- Payment history tracking
Why it matters:
Ensures smooth financial transactions and improves revenue management.
📊 Customer Portal (Self-Service Dashboard)
A customer portal provides policyholders with a centralized dashboard to manage all their insurance-related activities. Users can access policy details, track claims, download documents, and receive notifications.
Key features include:
- Real-time updates
- Easy navigation
- Personalized dashboards
Why it matters:
Enhances user engagement and reduces dependency on customer support.
🔐 Data Security & Compliance
Given the sensitive nature of health and financial data, security is a top priority. Health insurance software must comply with regulations such as HIPAA and GDPR to ensure data privacy and protection.
Security features include:
- Data encryption
- Secure authentication
- Access control mechanisms
Why it matters:
Builds trust and ensures legal compliance.
🔔 Notifications & Alerts
Automated notifications keep users informed about important updates such as policy renewals, claim status, and payment reminders. Alerts can be sent via email, SMS, or push notifications.
Why it matters:
Improves communication and ensures users never miss critical updates.
📁 Document Management System
This feature allows users and administrators to upload, store, and manage important documents such as policy papers, medical records, and claim-related files.
Why it matters:
Reduces paperwork and improves accessibility.
🎯 Final Insight
Core features form the foundation of a robust health insurance platform, enabling businesses to deliver efficient, secure, and user-friendly services while streamlining operations and improving customer satisfaction.
Advanced Features
To stay competitive in 2026, health insurance software must go beyond basic functionality and incorporate advanced technologies that enhance efficiency, personalization, and decision-making. These features not only improve operational performance but also deliver a superior user experience for both insurers and policyholders.
🤖 AI & Machine Learning
Artificial Intelligence plays a transformative role in modern health insurance platforms. AI algorithms can analyze vast amounts of data to automate underwriting, assess risks, and detect fraudulent claims. Machine learning models continuously improve accuracy by learning from historical data, enabling faster and more reliable decision-making. AI also powers chatbots and virtual assistants, providing instant support to users.
📡 Real-Time Data Processing & Analytics
Real-time analytics enables insurers to monitor claims, policy performance, and user behavior instantly. This allows businesses to make quick, data-driven decisions, identify trends, and optimize operations. Advanced dashboards provide actionable insights, helping insurers improve customer retention and reduce operational costs.
📱 Mobile App Integration
With the growing use of smartphones, mobile app integration is essential. Users can manage policies, submit claims, track status, and receive notifications directly from their mobile devices. This improves accessibility, convenience, and overall customer engagement.
☁️ Cloud-Based Infrastructure
Cloud integration ensures scalability, flexibility, and cost efficiency. It allows insurers to store and process large volumes of data securely while enabling remote access to the platform. Cloud solutions also support automatic updates, backup, and disaster recovery, ensuring uninterrupted service.
🔗 Third-Party Integrations
Health insurance software often integrates with external systems such as hospitals, pharmacies, wearable devices, and electronic health records (EHR). These integrations enable seamless data exchange, faster claims processing, and improved service delivery.
🔐 Advanced Security & Compliance
Security is critical in handling sensitive health and financial data. Advanced features include end-to-end encryption, multi-factor authentication, and role-based access control. Compliance with regulations like HIPAA and GDPR ensures data privacy and builds trust among users.
🧠 Personalization & Customer Experience
Modern platforms use AI to deliver personalized recommendations, policy suggestions, and health insights. This enhances user engagement and helps insurers offer tailored services based on individual needs.
🎯 Final Insight
Advanced features empower health insurance software to become intelligent, scalable, and user-centric, enabling businesses to deliver efficient services while staying ahead in a competitive digital healthcare landscape.
Development Process
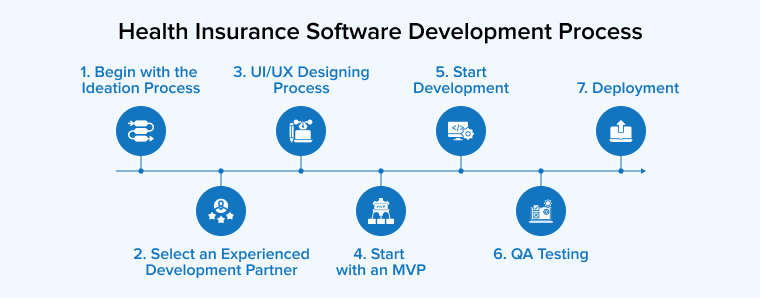
Developing health insurance software is a complex and highly regulated process that requires careful planning, secure architecture, and continuous optimization. Since these platforms handle sensitive medical and financial data, each stage must focus on compliance, scalability, and user experience.
🔍 Step 1: Requirement Analysis
The process begins with understanding business goals, user needs, and regulatory requirements. This includes identifying key functionalities such as policy management, claims processing, and customer portals. Stakeholders, including insurers and healthcare providers, are consulted to define clear use cases and workflows.
Why it matters:
A well-defined requirement phase reduces risks and ensures the final product aligns with business objectives.
🧩 Step 2: Planning & System Architecture
In this phase, developers design the software architecture and select the appropriate technology stack. Decisions are made regarding cloud infrastructure, database systems, and security frameworks. Compliance requirements such as HIPAA or GDPR are also incorporated into the design.
Why it matters:
A strong architecture ensures scalability, performance, and long-term sustainability.
🎨 Step 3: UI/UX Design
Designers create intuitive and user-friendly interfaces for both customers and administrators. Wireframes and prototypes are developed to visualize user journeys such as policy purchase, claim submission, and tracking.
Why it matters:
A seamless user experience improves engagement and reduces operational friction.
💻 Step 4: Development
This is the core phase where the application is built. Frontend developers create user interfaces, while backend developers build APIs, databases, and business logic. Integration with third-party systems such as hospitals, payment gateways, and analytics tools is also implemented.
Why it matters:
Ensures the system is functional, secure, and capable of handling real-world operations.
🧪 Step 5: Testing & Quality Assurance
Comprehensive testing is conducted to ensure reliability and security. This includes functional testing, performance testing, and security audits to identify vulnerabilities. Special attention is given to data protection and compliance validation.
Why it matters:
Prevents system failures and ensures a smooth user experience.
🚀 Step 6: Deployment
The software is deployed on cloud or on-premise infrastructure. Configuration of servers, databases, and security protocols is completed before launching the platform for users.
Why it matters:
Ensures a stable and secure launch environment.
📈 Step 7: Maintenance & Updates
Post-launch, continuous monitoring, updates, and performance optimization are essential. New features, bug fixes, and compliance updates are regularly implemented to keep the system up-to-date.
Why it matters:
Ensures long-term success, scalability, and adaptability.
🎯 Final Insight

A well-structured development process ensures that health insurance software is not only functional but also secure, compliant, and future-ready, enabling businesses to deliver efficient and reliable services in a competitive market.
Required Team Structure
Developing health insurance software requires a cross-functional team with expertise in healthcare regulations, secure software development, and scalable architecture. Since these platforms handle sensitive patient and financial data, assembling the right team is critical to ensure compliance, performance, and reliability.
👨💼 1. Product Manager (Strategic Lead)
The Product Manager defines the product vision and ensures alignment with business goals.
Key responsibilities:
- Define roadmap and feature priorities
- Coordinate between stakeholders and teams
- Monitor KPIs such as user engagement and system performance
Why it matters:
Ensures the product delivers real value and meets market demands.
📊 2. Business Analyst (Requirement Specialist)
The Business Analyst translates business needs into technical requirements.
Key responsibilities:
- Gather and document requirements
- Analyze insurance workflows
- Define use cases and user journeys
Why it matters:
Prevents miscommunication and ensures smooth execution.
💻 3. Frontend Developers (UI Experts)
Frontend developers build user interfaces for web and mobile platforms.
Key responsibilities:
- Develop responsive dashboards
- Integrate APIs
- Ensure seamless user experience
Why it matters:
Improves usability and customer satisfaction.
⚙️ 4. Backend Developers (Core Engineers)
Backend developers handle server-side logic and system architecture.
Key responsibilities:
- Build APIs and microservices
- Manage databases
- Implement business logic
Why it matters:
Ensures system scalability and performance.
🎨 5. UI/UX Designer (Experience Creator)
Designers create intuitive and user-friendly interfaces.
Key responsibilities:
- Design wireframes and prototypes
- Optimize navigation and workflows
Why it matters:
Enhances user engagement and adoption.
🧪 6. QA Engineer (Quality Assurance)
QA engineers ensure the platform works flawlessly.
Key responsibilities:
- Perform functional and security testing
- Identify bugs and performance issues
Why it matters:
Ensures reliability and reduces risks.
☁️ 7. DevOps Engineer (Infrastructure Expert)
DevOps manages deployment and scalability.
Key responsibilities:
- Set up cloud infrastructure
- Implement CI/CD pipelines
- Monitor performance
Why it matters:
Ensures smooth deployment and uptime.
🔐 8. Security & Compliance Specialist
Security is critical in health insurance systems.
Key responsibilities:
- Ensure HIPAA/GDPR compliance
- Implement encryption and access control
- Conduct security audits
Why it matters:
Protects sensitive data and builds trust.
📊 9. Data Analyst (Insights Expert)
Data analysts help optimize operations.
Key responsibilities:
- Analyze user and claims data
- Generate insights and reports
Why it matters:
Supports data-driven decision-making.
🎧 10. Customer Support Team
Provides post-launch assistance to users.
Key responsibilities:
- Resolve issues
- Handle queries
- Collect feedback
Why it matters:
Improves user satisfaction and retention.
🎯 Final Insight
A well-structured team ensures that health insurance software is secure, scalable, and compliant. Investing in the right talent is essential for building a reliable platform that meets the evolving demands of the digital healthcare ecosystem.
Monetization Methods
Health insurance software offers multiple revenue opportunities by leveraging flexible business models that cater to insurers, healthcare providers, and third-party stakeholders. In 2026, companies are increasingly adopting diversified monetization strategies to ensure consistent revenue while delivering value-driven services.
💰 Subscription Model
The subscription-based (SaaS) model is one of the most popular approaches. Businesses charge clients on a monthly or yearly basis to access the platform. Pricing can vary depending on the number of users, features, or data usage. This model ensures predictable recurring revenue and allows providers to continuously update and improve the software without requiring large upfront investments from clients.
📦 Licensing Model
The licensing model is ideal for enterprises that require customized solutions. Companies can offer on-premises or dedicated software licenses with one-time fees, along with additional charges for maintenance and upgrades. This approach is highly profitable for large-scale deployments and long-term enterprise contracts.
📊 Data Analytics Services
Health insurance platforms generate valuable data that can be transformed into actionable insights. By offering premium analytics services, businesses can help insurers with risk assessment, claims analysis, and customer behavior tracking. Advanced reporting tools and dashboards can be monetized as add-on features.
🌐 API Monetization
APIs enable seamless integration with hospitals, pharmacies, and third-party healthcare systems. Companies can charge partners for API access based on usage or subscription plans, creating an additional revenue stream while expanding the platform’s ecosystem.
💼 Consulting & Customization
Many organizations require tailored implementations and system integrations. Offering consulting, customization, and onboarding services allows businesses to generate additional income while ensuring clients get solutions aligned with their specific needs.
🎯 Final Insight
By combining subscription, licensing, analytics, and service-based models, health insurance software providers can build a scalable and sustainable revenue strategy in a competitive digital healthcare market.
Additional Section: Estimated Cost
The cost of developing health insurance software varies significantly based on factors such as feature complexity, technology stack, level of customization, compliance requirements, and the development team’s location. Since health insurance platforms must handle sensitive data and comply with strict regulations like HIPAA or GDPR, development costs are typically higher than standard applications.
💸Cost Breakdown
- MVP Development ($25,000 – $70,000)
A Minimum Viable Product (MVP) includes essential features such as user registration, policy management, basic claims processing, and a simple dashboard. This is ideal for startups or businesses looking to validate their idea quickly and enter the market with minimal investment. - Mid-Level Solution ($70,000 – $150,000)
A mid-level platform includes advanced features like automation in claims processing, payment integrations, analytics dashboards, and mobile app support. It offers better scalability, improved user experience, and enhanced security features. - Enterprise-Grade Solution ($150,000 – $400,000+)
Enterprise solutions are highly scalable and customized platforms designed for large insurance providers. They include AI-driven analytics, fraud detection systems, real-time data processing, third-party integrations (hospitals, pharmacies), and advanced security protocols. These systems also require compliance with strict regulatory standards.
⏱️ Development Timeline
- MVP: 3–5 months
- Mid-Level Product: 5–8 months
- Full-Scale Enterprise Solution: 8–12+ months
📊 Key Cost Factors
- Feature complexity and customization
- Integration with third-party systems (EHR, payment gateways)
- Security and compliance requirements
- UI/UX design complexity
- Development team size and expertise

🎯 Final Insight
Investing in health insurance software is a long-term decision that directly impacts operational efficiency and customer satisfaction. While initial development costs may seem high, the return on investment is significant through automation, reduced errors, and improved service delivery. Choosing the right development approach and prioritizing scalable architecture can help businesses optimize costs while building a future-ready insurance platform.
Conclusion
Health insurance software development is transforming the insurance industry by enabling automation, improving customer experience, and ensuring compliance. As digital transformation accelerates, insurers must invest in advanced technologies such as AI, cloud computing, and analytics to stay competitive.
The future of health insurance lies in personalization, automation, and real-time decision-making. Businesses that adopt these innovations early will gain a significant advantage in the evolving healthcare ecosystem.
FAQs
It is a platform that manages policies, claims, billing, and customer interactions.
It ranges from $25,000 to $400,000+ depending on complexity.
3–12 months depending on features.
AI, cloud computing, APIs, and secure databases.
Automation, efficiency, improved customer experience, and reduced costs.


